Hello Friends. Today I want to share all about my DIEP flap surgery. Last week, I shared that I would be dedicating my Monday’s to sharing my triple -negative breast cancer journey. I spent my Monday’s at the Mayo Cancer Clinic in Phoenix from October 2017- May 2018. Every chemo treatment, lab draw, scan and visit with the oncologists and surgeons all fell on that magical Monday.
This week I want to dive in a little further with the Breast Reconstruction options. Having had my diep flap surgery just three weeks ago today, I am feeling like I can see light at the end of the tunnel. This third surgery was just six weeks after the second. At a time I should almost be healed. I developed an area of fat necrosis under the incision. It had to be opened and drained. Not able to close on it’s own, I needed to have the 3rd surgery to fully clean out the area and close the incision again. So, although it’s only been 3 three weeks it has been 9 and I am ready to be back at “all the things.” Trust me, looking around this weekend, I am needed.
To recap, my first surgery was just a month after my last chemotherapy treatment. I opted for a double mastectomy. I only had the cancer in my left breast, but I knew the mental head game I would put myself through in worry if I didn’t remove the right. Following the mastectomy, I had immediate breast reconstruction where they placed textured gel implants above the muscle. They were firm if not brick hard, they were too large for my frame and little skin coverage I had to hold them. They caused intense pain about 2-3 months after my surgery. Being told that it was normal and I could expect that for months to come. The pain was different though. It was a burning and I couldn’t lay on my side because they felt like they were cutting me. The pain and discomfort never faded, but rather stayed constant. I also began having bone pain in my hands and feet. There were many odd coincidental symptoms that I can look back and see how unrelated they may have looked to the doctors. However, once those implants were removed there were several symptoms that immediately were removed as well.
Knowing all the risks requires your own research.
There is a real rare cancer that women are developing from these types of implants. Breast Implant Associated ALCL attacks the immune system and many women who trust their surgeons to remove the cancer during mastectomy are being subject to a new cancer with the use of these implants. FDA approved or not, it’s yours to know before deciding. You can read more about that here. I am not a doctor, I do not have an expert opinion to add to this. Just do your research and make sure you advocate for yourself. Every doctor should/will tell you that you are your best advocate. No one knows their body better than you.
Exploring New Options
When we moved home to Oklahoma City the first of December, it was because my husband’s father was very ill. So grateful we were able to spend the last month of his life with him. However, just leaving Phoenix with concerning lab results, I was immediately seen by a new oncologist. Dr. Theobald was my lifesaver, literally. She acknowledged my pain I was in, before I could tell her. She told me about the options I had available to pursue. She gave me the name of the “only” surgeon she worked with and that I should see. But she also told me about the healing time and the things I needed to consider before I went to see him. It was a decision I would need to fully explore and decide if it was worth the downtime involved.
With the pain only becoming worse, I decided to meet with Dr Masters the beginning of February. Simply, cannot express the sheer gratitude for an amazing new breast surgeon. Where I, like the majority of breast cancer patients, didn’t know all my options for the actual surgeries. I have always been diligent in choosing a Board Certified Surgeon. If you need help in your research, this link will open in a separate page to help you find out more. ( All of the highlighted text have outgoing links so you can keep this post open and easily navigate between all the information.)
When we met, we discussed how my initial surgery was not right for me. He was extremely honest and upfront with all the reasons. Interestingly, I found out he was also a student and mentored under my first surgeon in Texas in years prior. His amazing nurse took many pictures and he came back in and presented me with only 2 options. Truly, one wasn’t an option- the implants must come out. They had failed due to capsular contracture. The pain I was experiencing was real and he didn’t overlook it for a moment. Also, I was at a higher risk for developing ALCL with everyday that the implants remained.
The next option had me a lot scared. Suggesting a DIEP flap and a PAP flap. Taking the time to thoroughly explain what each acronym stood for, what each procedure entailed, how many he had performed, how many the group had done collectively, their success rate, and all of the risks associated with each. This flap surgery was removing my skin, fat, blood vessels and tissue from a “donor site” of my abdomen and thigh area and transferring it all to rebuild the breasts. He explained my fit as a candidate, what I could realistically hope to achieve, and what I shouldn’t expect to achieve.
I had to not just understand, but articulate everything he had spoken to me in detail back to him. All the while he illustrated and wrote it out for me to visually see and take home. Beyond the actual surgery details, this also meant understanding my part in remaining a candidate. Which for me, meant I had no weight to lose. Prior to chemotherapy, I was very thin. I wore a size 0 or even kids 14 on most days and weighed under 135 pounds. Thankfully, my taste buds were attacked during chemotherapy and I craved all things carbs and Cane’s. It allowed me to even be a candidate for this procedure. I had gained over 20 pounds during chemo, but had lost about 10-12 pounds of that weight at the time I met with Dr Masters.
Given that the surgery was heavily relying on my fat tissue to build my breasts, I had to be very realistic with my expectations and choices. Not having a lot of fat, meant I couldn’t expect to have larger breasts. I took that information home and discussed with my husband and did a little bit of research.
There are only a few surgeons in the US performing the more difficult level of donor site surgeries and I was lucky enough to have not one, but two of them!!
Beyond finding a qualified surgeon, you want to be sure you qualify as a candidate. You want to be sure you are aware of all the risks that pertain to you and your body. Asking your surgeon to fully detail all of these things is absolutely important for you both.
Things to ask your surgeon if MICROsurgery is what you are exploring.
Below are important questions and they should be met with a high level of care and concern, not ego. MICRO-VASCULAR surgery is very intricate and complicated and you want to have the very best operating on you for your success.
Are you a board certified and fellowship trained in microsurgery? How many DIEP flaps have you performed? What is the success rate for your practice on this specific type of surgery. How many surgeons will be in on my case at the time of surgery? Am I a good candidate for this type of surgery? What risks could I specifically encounter? Is there anything I should consider changing in my habits to achieve better results?
When considering this type of surgery, it is vital that you are realistic and honest with yourself about your goals and what you are hoping to achieve.
After a lot prayer and careful consideration, the following week I made the call to agree to surgery. I was already sent for the CT scan needed to map all of my blood vessels and prepare the surgeons for my case in the event that I would agree. The following day, I received the call that surgery would be in 2 weeks. I went in for preop that afternoon. Where I would learn that my inner thighs would not give them enough to undergo the additional healing required. So I would need to decide if having a small round saline implant to increase the volume would be important to me.
In this, my only objective was to not have a sunken in chest. There is not one thing that will give me back all that cancer has taken from me. So having perfect boobs- it just wasn’t high on my priority list. I have been sick and a patient for 3 years and I am over it all. I want to LIVE- and the size of my breasts don’t dictate how I live.
Given the size of my breasts was never a concern for me. The morning of surgery, during the drawings and mapping, both doctors decided to veto the addition of the small implant. They would continue on with a nipple area, but it would be tattooed rather than 3D. Another plus to me.
At Mayo, I was always a patient ID number. Continuing care is not something that they were built to offer. If I stress anything, I want it to be- that in your advocating you also find a doctor who sees you. Who really hears you and can give your the space to feel comfortable in your conversations. Who makes you comfortable enough to be honest with you as well. Being in a plastic surgeons office, can heighten your awareness of all your imperfections. It can make you feel vulnerable. But it was in the area of dialog that being comfortable enough to express, I am a 46 year old mama, I never aspired to be a boob model, so size isn’t my end game but living is. Allowed, Dr. Masters and Dr. Habash to take in my whole self, autoimmune issues, and do what was best for me. Perfect!!
After Surgery
My surgery required 3 days in the hospital, where they would monitor the blood flow of my new tissue. This was the biggest risk for failure in this surgery and usually it will fail immediately, if at all. What provides the best quality of life and most natural look and feel for your breast is also the largest area of risk. If adequate blood flow supply is not achieved, the new tissue will die in the process. I had sensors that monitored this very closely. My blood flow numbers were some of the highest the nurses had seen. That filled me with great hope. The sensors I wore filled my visitors with lots of giggles.
Adorned with 2 drains from my breasts and 2 drains from my abdomen. The breast drains would be removed before I went home and the abdominal drains would be removed in follow up appointments.
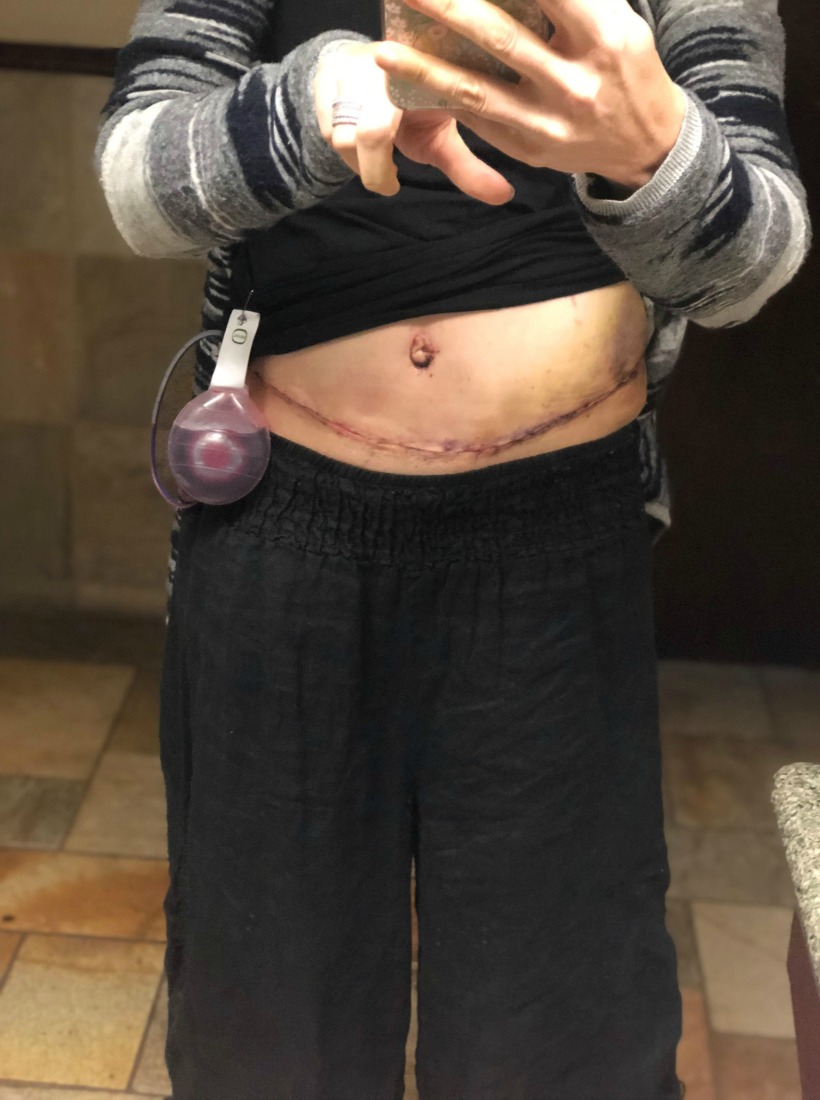
Even with knowing all the risks, all the restrictions and why’s… it didn’t really adequately prepare me for the physical pain I would feel in the abdominal area. Being cut open from hip to hip, was not an easy matter. My pain medication regimen was really important. I know that it will be different for all patients. I was very successful with ibuprofen and tylenol. And during the first two weeks I took Gabapentin, something that I also took during chemo for neuropathy. The side effects are atrocious but the benefits outweighed them.
Rest and downtime are two of my least favorite words and no one would ever use them as virtue descriptors about me. However, both are absolutes for this kind of surgery. You need to know it going in and you need to adhere to it during the process. Your healing will not go faster pushing through pain. Pain is there to remind you how little you are supposed to be doing.
I had weekly and almost daily visits. The way I felt was far better than how I should. There was no pain in my breasts, range of motion was greater than it had been in years. My abdominal strength was amazing. Standing up straight helps back pain but puts stress on abdominal incisions. With everything moving forward so quickly, I had been given instructions on compression. And that was so important for swelling and promoting healing, but also the key to slowing me down. Staying slightly hunched over, for longer than my body wanted to, was something I had to really focus on. Especially after the initial surgery. I was sitting up and getting up so well and walking straight up… all things I was unaware of hurting my healing.
I shared my surgery on my facebook page and I am so glad that I did. Meeting a new friend who was just a month ahead of me and it was so incredibly wonderful to be able to walk through it with someone who fully understood what I was experiencing. We have been able to bounce things off each other, encourage one another, and pray for each other in the hard and difficult times. I don’t think I could have gone through this without her!! Thank you Diana!!
Next week, I will share more about the healing process, complications I had coming home, and the third surgery to repair. There is so much information above and I know it can be daunting and overwhelming. And so sharing everything that you might have questions about here in brief doesn’t really help you in your search for answers. I want to be sure to give you a real glimpse into what those 8 weeks look like. Why it’s important to listen to your body, to find people who have gone before you, and just a deeper view into this process.
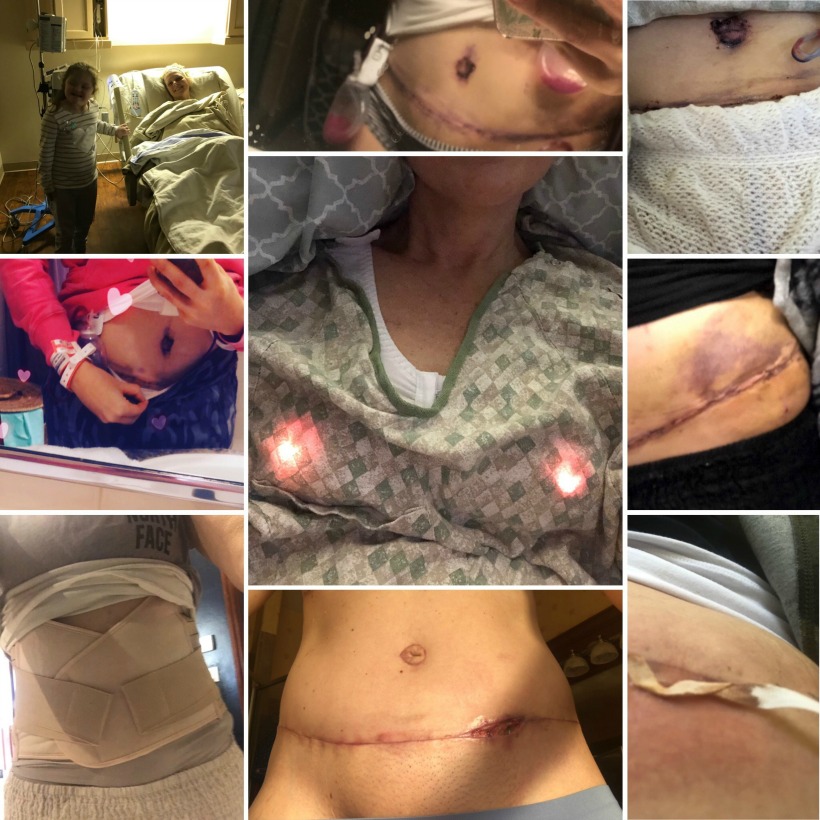
[…] the way. I planned to before today- but I had a few really hard weeks of recovery after this last breast reconstructive surgery. So come back- even better subscribe today and be the first to see the […]
I have enjoyed reading about your surgery. I had a friend that had the same thing. She was out of work for a long time. but it paid off. Thanks for sharing!
Thank you Susan. The recovery was indeed a lot longer than described. I pray your friend is doing well now!!
I am in the process of preparing for diep flap surgery, probably in March. I have been trying to get as much information as possible. I am scared but I know I have to move forward. I appreciate your information and look forward to the reading your healing process, hopefully I can read that before my surgery.
Thanks,
Jill
Jill, I am so sorry I am just now seeing this comment. I have just recently started back blogging and launched a podcast (episodes are live within my blog portion of the website- vintagecharmrestored.com/blog. The rest of the site is just making it’s transition and I am trying to use my chemo brain to its fullest… lots of the tech stuff was stolen by chemo LOL. I hope that you are doing well and if you need anything please feel free to email me at vintagecharmrestored@live.com
Thank you so much for sharing your story . As I am preparing for my diep flap surgery in the coming month. How do u feel now with your scars/ have they lessened? Story was very informative!!
Thanks
Ericka
Thank you for sharing & describing everything so well. You’ve validated my decision not to do implants. I had DIEP surgery in Sept 2022 & will have the liposuction part done in the spring. I had heard from others about how painful it will be but I’m ok with it & hoping my boobs will end up looking better than they now do. I feel like a Frankenstein with all the scars & stitches. Just wanted to thank you & let you know you are appreciated!